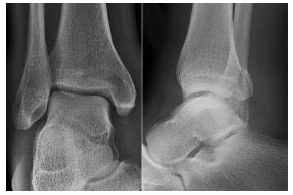
This report presents the case of a distal fibula non-union in an 8-year-old girl who was initially conservatively treated but who then required surgical remediation. įortunately, the occurrence of non-union consequent to a pediatric fibula fracture is rare in the population but, is significant to the affected individual. However, the incidence of non-union increases with bone infections and with premature, and repeated manipulation. These traumas associated with distal fibula fracture are accompanied by a very low incidence of long-bone non-union (0 to 1.7%). Of these fractures, between 3 and 12% are distal fibula fractures which are most commonly associated with ankle sprains, the majority of which are sports-related, and which represent than one-third of children’s sporting injuries. In the pediatric population, 15% of all the fractures involve the physis in different ways. Surgical treatment as well as talar chondral evaluation should be taken into consideration in the treatment of pediatric distal fibular nonunion. This case report illustrates the necessity of particularly meticulous evaluation of pediatric post-traumatic ankle pain. Surgical excision of the fragment and chondroplasty was performed and resulted in an excellent clinical outcome. We report the case of an 8-year-old girl with an epiphyseal distal fibula fracture complicated with a symptomatic non-union associated with the chondral flap of the talar dome after conservative treatment. However, even in clinically stable ankles, subsequent pain arising from fracture site could suggest non-union, thereby necessitating reexamination and possible secondary treatment. Historically, the most common treatment of a lateral malleolus fracture after an ankle sprain is conservative, which usually leads to fracture union. To do this, emergency physicians need to employ stress radiographs to assess the stability of the ankle joint.In children, fracture non-union is uncommon yet, curiously, non-union of distal fibula fractures are rarely reported. 3 For this reason, assessing deltoid ligament integrity is of critical importance in determining the stability of an ankle fracture. 5Ĭlinical signs such as medial ankle pain, swelling, and ecchymosis are not reliable in identifying a deltoid ligament injury. 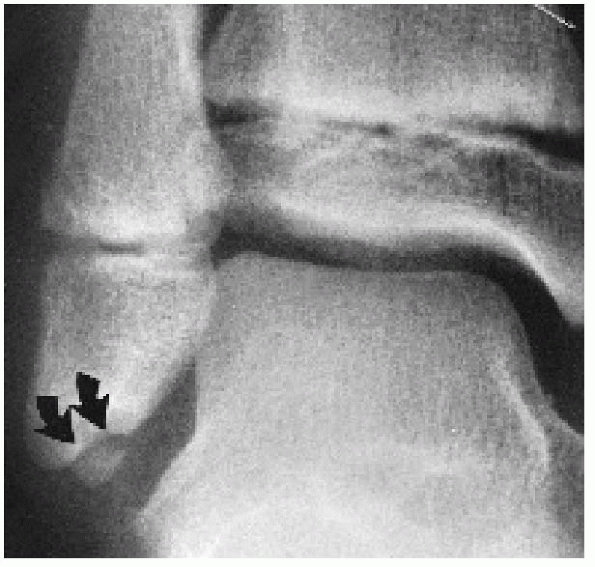
4 In what appears as an otherwise isolated Weber B fibular injury, a tear of the deltoid ligament can be considered “equivalent to a medial malleolar fracture,” qualifying the fracture mechanically as unstable, thus requiring operative management. A talar shift of 1 mm results in a 42 percent decrease in tibiotalar contact area, which can lead to significant increases in contact stress. The deltoid ligament, which runs from the medial malleolus to the calcaneus, talus, and navicular bones, plays a vital role in maintaining correct talus positioning. With Weber B fractures, the stability of the ankle joint depends on injury to the tibiofibular ligaments and the deltoid ligament. Any bi- or trimalleolar fracture should be considered unstable because of the disruption of the bony architecture on both the medial and lateral side of the joint. Unstable ankle fractures are one of the primary indications for orthopedic referral. In general, most stable ankle fractures can undergo nonoperative management by a primary care physician. The primary consideration regarding need for operative management of a closed ankle fracture is stability. The focus of this article is to help emergency physicians choose the proper method for determining that stability. 3 These type B fractures are sometimes stable, and patients can ambulate on them as tolerated in other cases, they are unstable and require open reduction and internal fixation (ORIF). Weber B fractures occur at the level of the tibiofibular ligaments, just above the talar dome, and happen primarily through a mechanism of ankle supination and external rotation (SER). Weber C fractures are almost always unstable and require surgical intervention. Weber C fractures are above the ankle joint and are associated with a syndesmotic injury. Injuries to the distal fibula, below the talar dome, are classified as type A and are stable fractures. Tips for Diagnosing Occult Fractures in the Emergency DepartmentĮxplore This Issue ACEP Now: Vol 39 – No 04 – April 2020.Tips for Catching Commonly Missed Ankle Injuries.Tips for Managing Suspected Occult Fractures.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
